
What is Necrotizing Enterocolitis?
Necrotizing enterocolitis, or NEC, is a common gastrointestinal emergency affecting newborns. It is more common in premature infants, but can develop in full-term infants as well. NEC is characterized by necrosis of the mucosa lining…
Necrotizing enterocolitis, or NEC, is a common gastrointestinal emergency affecting newborns. It is more common in premature infants, but can develop in full-term infants as well.
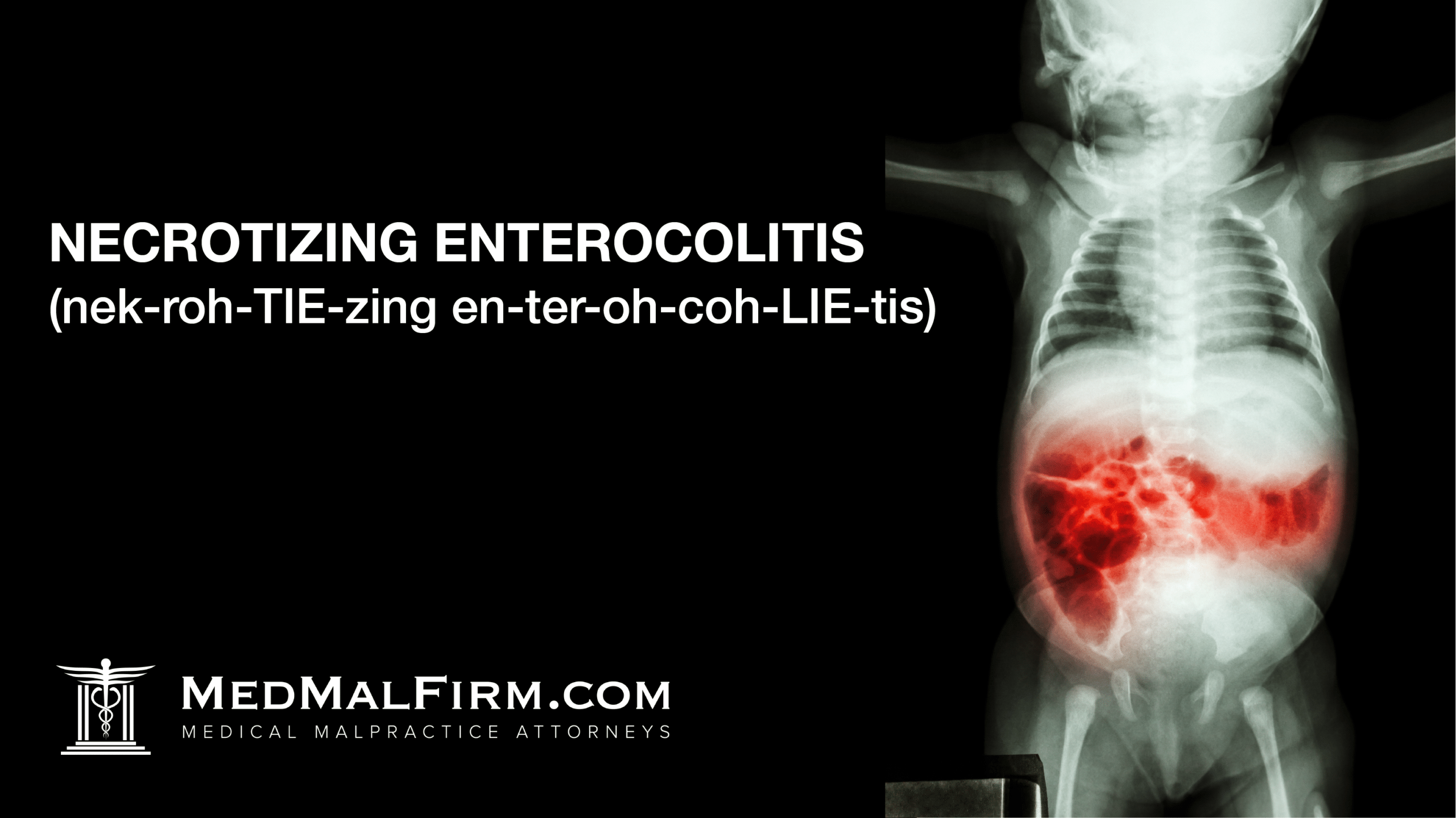
NEC is characterized by necrosis of the mucosa lining the intestines. That means, the soft lining on the intestines becomes inflamed and begins to die. The result is bacteria, gases and intestinal fluid leaking into the bowels and/or abdomen. Infants can then suffer painful symptoms, possible surgery, sepsis or even death.
NEC is gaining attention in the United States due to research showing that using cow’s milk-based infant formulas increases the risk of infants experiencing the disease. In fact, cow’s milk-based formulas have been positively linked to NEC, and are considered one of the primary risk factors for NEC.
What is Necrotizing Enterocolitis?
The exact cause of NEC is unknown, but experts believe it is the result of a combination of:
- Immature intestinal tract
- Immature immune system
- Triggers that disrupt the normal intestinal microbiome
- Increase in the growth of pathogenic bacteria
- Exaggerated inflammatory response
Infants who are premature and low birth weight are most susceptible to NEC because they have very vulnerable and immature immune and intestinal systems. The more premature and the lower the birth weight, the greater the risk of NEC. This is especially true among infants who are fed cow’s milk-based formulas.
The immature digestive tract in premature infants has not developed to the point where their bodies can completely absorb and digest nutrients. Because of that, milk products may ferment or not digest properly. This causes injury to the lining of the intestines.
Some co-occurring medical conditions may also increase the risk of NEC, including chorioamnionitis. Chorioamnionitis is inflammation of the fetal membranes caused by a bacterial infection. It is a possible risk factors for developing NEC, generally alongside risk factors like prematurity.
Complications of NEC include intestinal perforation and peritonitis (inflammation of the lining of the abdominal cavity). Sepsis occurs in 20-30% of NEC cases. This overwhelming response to an infection causes inflammation throughout the body, including the organs. Sepsis often leads to organ failure and septic shock. Septic shock further damages organs and tissue. It is fatal in around 50% of cases.
Importance of Human Milk Feeding
Whenever possible, human milk should be given to newborns, especially those born prematurely. Human breast milk contains components not found in formulas, such as:
- Lactoferrin
- Lysozyme
- Oligosaccharides
- Cytokines
- Acetylhydrolase
- Glutamine
- Antioxidants
- Epidermal growth factors (EGFs)
These components are what helps develop the intestinal and digestive tracts and microbiomes. Studies suggest that human donor milk, rather than formula, decreases the risk of NEC.
Over 90% of infants who have NEC have been fed non-human milk formulas.
Human milk contains important nutrients that help:
- Protect the baby from diseases and digestive problems
- Promote immune system development and health
- Enhance the baby’s intestinal motility
- Lower the baby’s gastric pH
Of course, it is not always possible for a new mother to breast feed, and in such cases, experts recommend using donor milk. Donor milk is available in most neonatal intensive care units (NICU), and the donor and her milk go through an intense screening process.
If a new mother is unable to breastfeed, or is unable to produce enough milk, donor milk is a great alternative.
Diagnosing and Treating NEC
Doctors generally diagnose NEC after they discover abdominal distention or blood in the baby’s stool. Sometimes, NEC is not diagnosed until the condition has advanced to the point of sepsis, which causes additional symptoms including fever, lethargy, apnea and metabolic acidosis.
Doctors diagnose NEC by performing a thorough medical examination. They may also order an ultrasound and x-rays of the baby’s abdominal area. Imaging tests allow doctors to see what is happening inside the baby’s body, including blood flow, bowel wall thickness and the presence of perforation if one exists.
Once doctors confirm the diagnosis, they should initiate treatment immediately. Treating NEC includes one or more of the following techniques:
- Temporarily halting all feedings
- Inserting a tube through the mouth or nose to remove fluid and air from the stomach and intestines
- Using IV fluids to replace feedings and provide hydration
- Administering antibiotics to prevent or treat infection
- Periodic follow-up imaging tests to monitor healing
- Surgery
Non-surgical treatment is effective in around 75% of NEC cases. In severe cases, surgery may be necessary and emergent.
Timely diagnosis and immediate treatment increases the baby’s likelihood of surviving NEC. Sadly, the mortality rate is around 20-30%.
Can NEC be Prevented?

There are several ways that healthcare providers attempt to prevent NEC in the first weeks of life, such as:
- Preventing premature birth
- Using only human milk
- Using antenatal corticosteroids
- Avoiding prolonged or unnecessary antibiotics
- Avoiding histamine [2] blockers, which reduce gastric acidity
- Using a standardized feeding protocol, such as administering colostrum
Research does not support use of probiotics or immunoglobulins as an effective means of preventing NEC.
Does Your Child Have NEC?
NEC is a serious medical condition that has a tremendous impact on your child and family. At MedMalFirm.com, our attorneys are currently investigating claims related to necrotizing enterocolitis caused by cow’s milk-based infant formulas. If your child was fed formula in a neonatal intensive care unit (NICU) and developed NEC, contact us today to learn more about your legal rights.
Find out if you qualify for compensation related to your child’s NEC by completing our online form, or by calling us at (877) 887-4850. A case review with one of our attorneys is completely FREE.
Sources:
- https://www.uptodate.com/contents/neonatal-necrotizing-enterocolitis-prevention?topicRef=5006&source=related_link
- https://www.uptodate.com/contents/neonatal-necrotizing-enterocolitis-management
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3628622/
- https://www.birthinjuryguide.org/birth-injury-types/chorioamnionitis/
- https://www.merckmanuals.com/professional/pediatrics/gastrointestinal-disorders-in-neonates-and-infants/necrotizing-enterocolitis
- https://necsociety.org/
