Retinopathy of Prematurity
Retinopathy of prematurity is a birth injury that affects around 15,000 newborns each year. ROP is the second-leading cause of blindness in the United States. Pregnant women and parents of premature newborns should be aware of ROP, the symptoms, monitoring and why immediate treatment is so crucial.
Some cases of ROP are due to medical negligence. Either the mother did not receive adequate prenatal care, or the infant’s healthcare team did not adequately monitor for ROP, diagnose or treat it in a timely manner. Sadly, these instances of negligence cause infants to suffer permanent eye damage or blindness.
Premature newborns require assessment and monitoring by an ophthalmologist to ensure immediate diagnosis and treatment.
If your premature newborn has ROP call us at (877) 887-4850 for a free case review or fill out the form below.
Find Out for FREE if You Qualify!
What is Retinopathy of Prematurity?
Retinopathy (ret-in-AH-puh-thee) of prematurity (ROP) is an eye disease that causes abnormal growth of the blood vessels in the eyes. Abnormal blood vessels grow into the retina or randomly into the eye, which can lead to vision loss or blindness.
Infants who are born prematurely may have a condition called retinopathy of prematurity, or ROP. ROP primarily affects infants born before 31 weeks of pregnancy. It is also more common in infants weighing less than 2.75 pounds, or 1,250 grams.
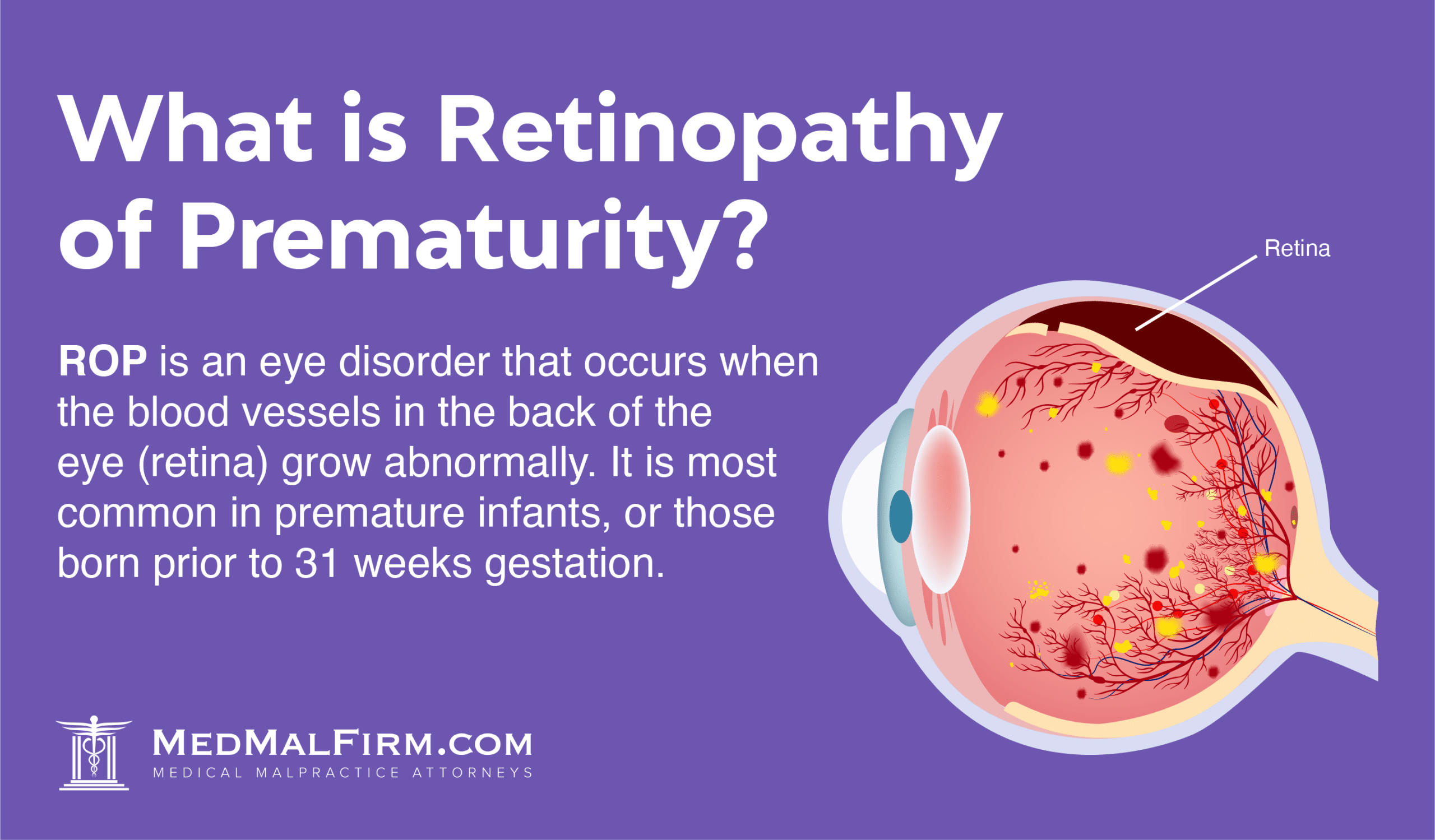
When blood vessels leak into the eye, it causes scarring on the retina. As these scars shrink, they tug on the retina, and can cause it to completely detach from the eye. The retina is a crucial part of vision, and detachment can cause permanent blindness.
How the Retina Develops
The blood vessels in the retina (the back of the eye) start to develop at around three months of pregnancy. They are generally fully developed by the time the infant is full-term. When infants are born prematurely, their eyes may not be fully developed, or may have abnormalities.
The blood vessels in the eye are incredibly fragile. Premature infants are at risk for blood vessels leaking into the eye, retinal detachment and even vision loss.
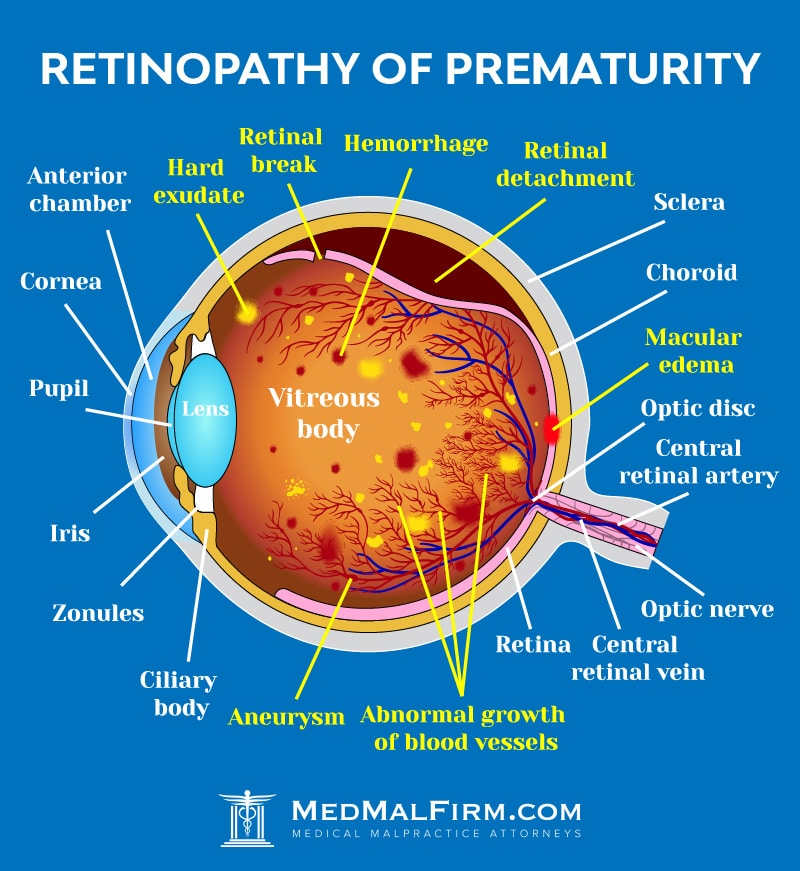
What Causes Retinopathy of Prematurity?
One possible cause for ROP is too much oxygen given to premature infants. Too much oxygen after birth can cause the vessels to grow abnormally. In recent years, experts have developed better ways to monitor oxygen levels, which can reduce the risk of ROP.
In addition to too much oxygen, experts believe the risk of ROP is much greater in infants who are significantly premature. Also, newborns with other medical problems are at a higher risk of developing ROP. Risk factors that experts believe may contribute to ROP include:
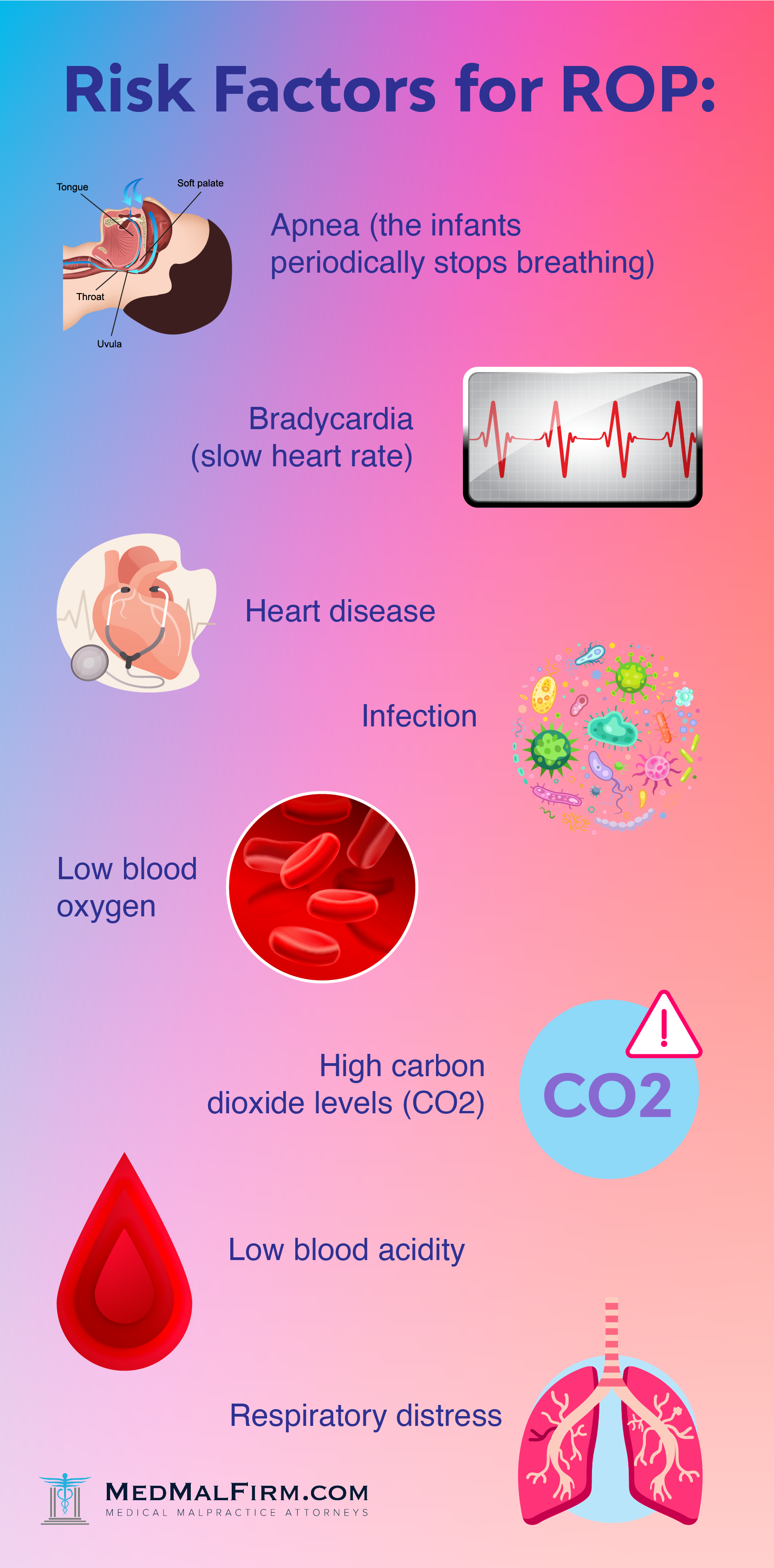
In developed countries like the U.S., there has been a decline in rates of ROP due to advances in care for premature infants. However, premature infants are still vulnerable to the risks of conditions like ROP and necrotizing enterocolitis, or NEC.
Diagnosing Retinopathy of Prematurity
Changes in the blood vessels in the eye cannot easily be seen just by looking at the eye. Instead, an ophthalmologist will need to conduct a thorough examination of your child’s eye to determine if he or she has ROP. This exam and any tests will generally take place 4-9 weeks after your baby is born, depending on his or her gestational age.
- Newborns born 27 weeks or later will generally have their first exam four weeks after birth.
- Newborns born prior to 27 weeks will have their first exam later.
Based on the exam, your doctor may then diagnose your child with one of the five stages of ROP, which are:
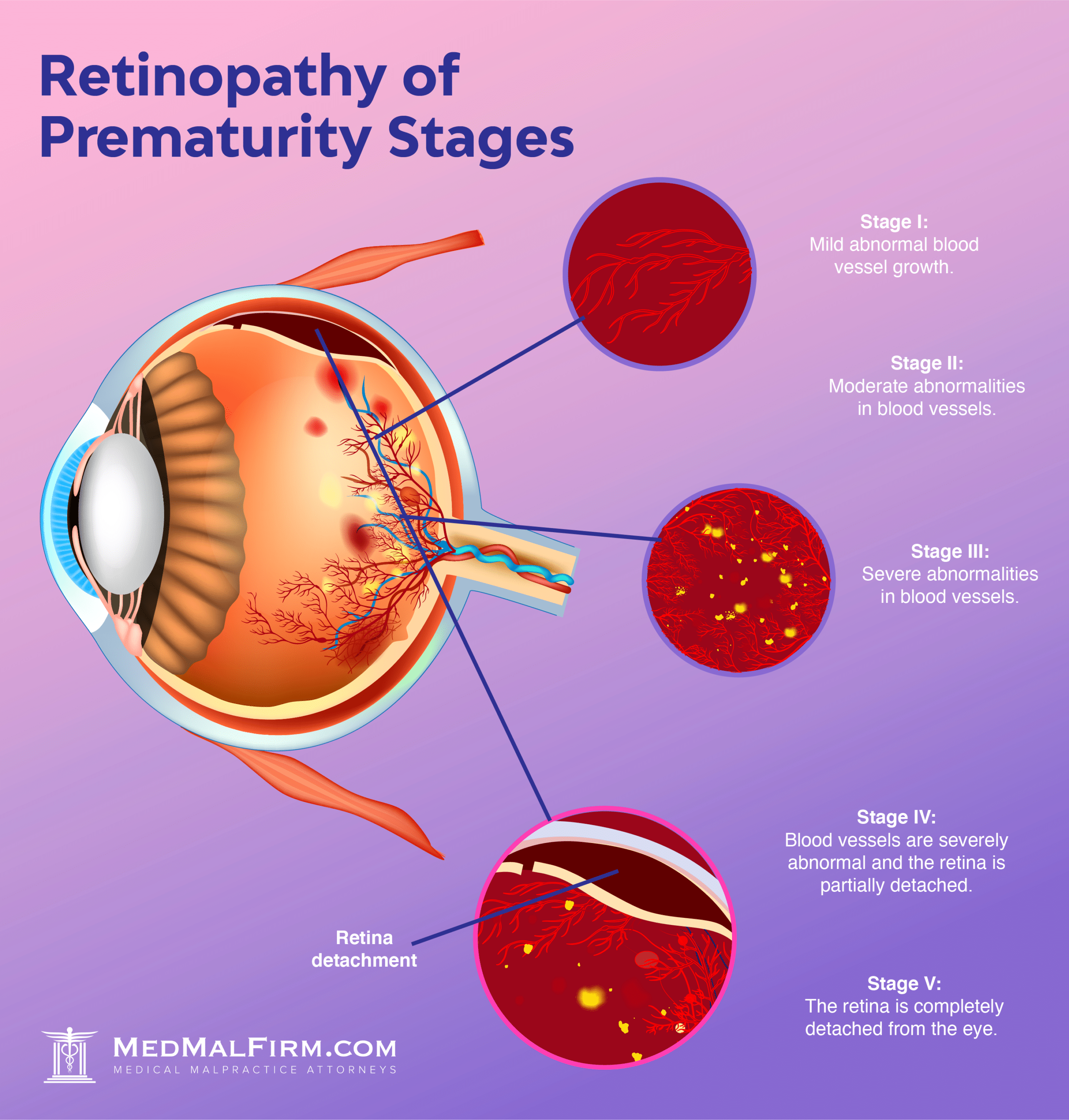
While mild or moderate ROP does not generally cause noticeable symptoms, severe cases can cause symptoms like:
- Crossed eyes
- Abnormal eye movement
- Severe nearsightedness
- The pupils are white in appearance (leukocoria)
Your child may have a diagnosis of “plus disease” when ROP is severe.
Retinopathy of Prematurity Treatment
If the first exam shows that the retinas have developed normally, then additional exams and treatment are usually not necessary. If the retinas are abnormal, then additional exams and treatment should begin.
Immediate treatment is imperative to preserving normal vision for infants with ROP. Treatment should begin within 72 hours of making the diagnosis. The most common treatment options for ROP are:
- Laser Therapy: Laser therapy burns away the periphery of the retina.
- Cryotherapy: Cryotherapy freezes small spots on the surface of the eye that overlie the periphery.
Both therapies kill destroy peripheral areas of the retina, which slows or reverses abnormal growth of blood vessels. Sometimes, this can cause damage to the peripheral vision of the infant. The goal, however, is to retain vision in the center or “straight ahead” areas of the eyes.
Severe stages of ROP or plus disease may require more invasive treatment, such as:
- Scleral Buckle: A scleral buckle is only used to treat stages IV or V ROP. It involves placing a silicone band around the eye to help the retina flatten against the back of the eye. The buckle is removed months or years later.
- Vitrectomy: A vitrectomy is only used for stage V ROP. The vitreous is removed from the eye, and is replaced with a saline solution. Once this is done, the scar tissue can be peeled away, and the retina can relax and flatten back against the eye wall.
Prognosis for Infants with ROP
With timely diagnosis and treatment, the prognosis for infants with ROP is generally good. Many infants recover from ROP with little or no treatment at all. However, the more severe the disease is, the more treatment and monitoring will be necessary.
Most infants who develop ROP have other medical problems associated with premature birth. The earlier the birth and the more severe the medical problems, the more likely it is that the infant will develop additional problems later in life. For infants with ROP, early eye disease can lead to vision problems or blindness later in life.
The key to preventing ROP is getting proper prenatal care and taking every opportunity to prevent premature birth. The key to reducing the risks associated with ROP is timely diagnosis and treatment when the infant does have the disease.
